Efficacy of rhTNFR: Fc in the Treatment of patients with Rheumatoid Arthritis
Rheumatoid arthritis (RA) is a chronic, progressive, and erosive disease, which is manifested with symmetric, polyarticular inflammation. Tumor necrosis factor alpha (TNF-α) plays a very important role in the pathophysiology of RA. However, TNF levels are found to increase abnormally in lesions of articular cavity of many patients or animal models. Furthermore, TNF-α generally works by binding to the receptors on the cell membrane, thereby causing death of target cells or aggregation of immune effector cells. Tumor necrosis factor alpha antagonist results in effective alleviation of the disease by decreasing inflammation and articular damage.
Disease-modifying antirheumatic drugs are the mainstay of treatment in patients with RA, as they prevent disease aggravation and delay articular damage. Methotrexate (MTX) is the first choice in RA treatment because of its good efficacy and safety profile. However, there are certain limitations associated with the use of MTX, such as liver damage, gastroenteric reactions and infection susceptibility.
The recombinant human tumor necrosis factor receptor:Fc fusion protein (rhTNFR:Fc) is a biotech product and a form of fusion protein produced by recombinant DNA technology. This protein is thought to block the interaction with TNF receptor on cell surface by binding specifically to TNF.
Introduction
Tumor necrosis factor alpha plays an important role in the pathological process of RA. In addition, rhTNFR:Fc is a kind of fusion protein produced by recombinant DNA technology, which can block the interaction with TNF receptor cell.
Objective and methods
A double-blind, randomized, multicenter study aimed to determine the efficacy and safety of rhTNFR:Fc in 238 patients with moderate or severe active RA for a period of 24 weeks. Among the total cases, 118 cases were included in the test group who received Etanercept subcutaneous injection treatment, and 120 cases were included in the control group who received oral MTX treatment. About 209 cases completed the study, which include 101 cases in the Etanercept group and 108 cases in the MTX group. Therapeutic efficacy was determined based on the American College of Rheumatology (ACR) criteria.
Efficacy Assessment
The efficacy was assessed by using the American College of Rheumatology ACR criteria (ACR20, ACR50 and ACR70).
The criteria for ACR20 : Improvement in tenderness/pain joints by 20% (28 joints) and improvement in at least 3 of the following 5 items by 20%.
- The visual analogue scale (VAS) score of joint pain assessed by the subjects
- The VAS score of general status of the disease assessed by the subjects
- The VAS score of general status of the disease assessed by the investigators
- Health assessment questionnaire
- Responding laboratories – Erythrocyte sedimentation rate and C-reactive protein
The criteria for ACR50 and ACR70 includes improvement in the responding rates of the above items for ACR20 by 50% and 70%, respectively.
Results
At 2 weeks
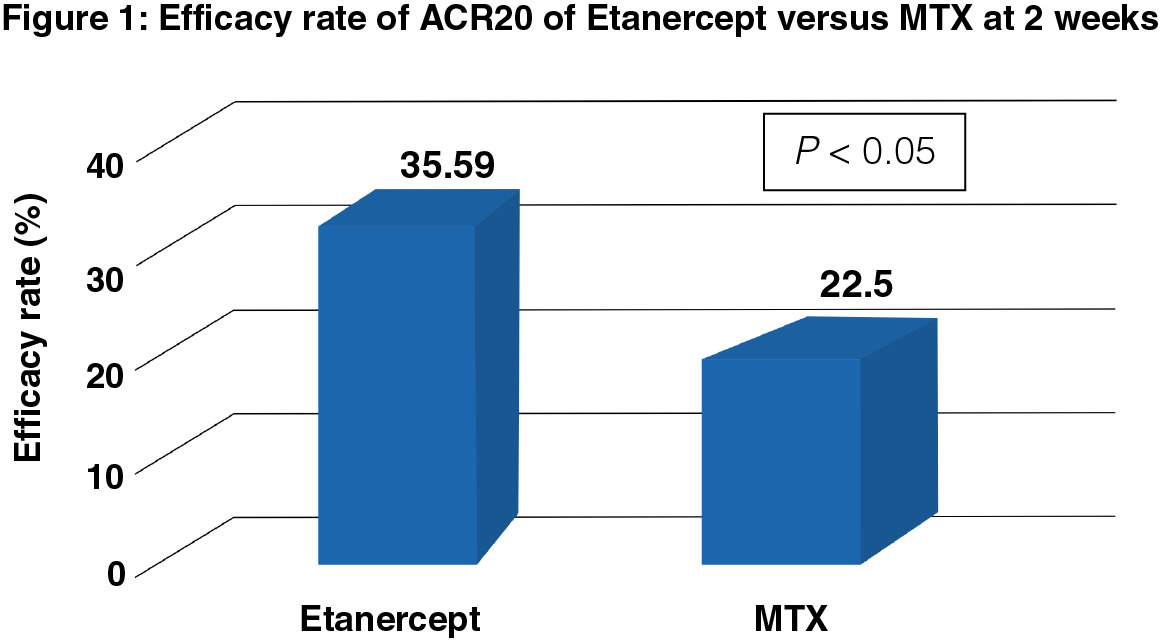
There was a significant difference in the efficacy rate of ACR20 of Etanercept and MTX (35.59% and 22.50%, respectively, P < 0.05) after 2 weeks, thus, indicating faster response with Etanercept compared to MTX (Figure 1).
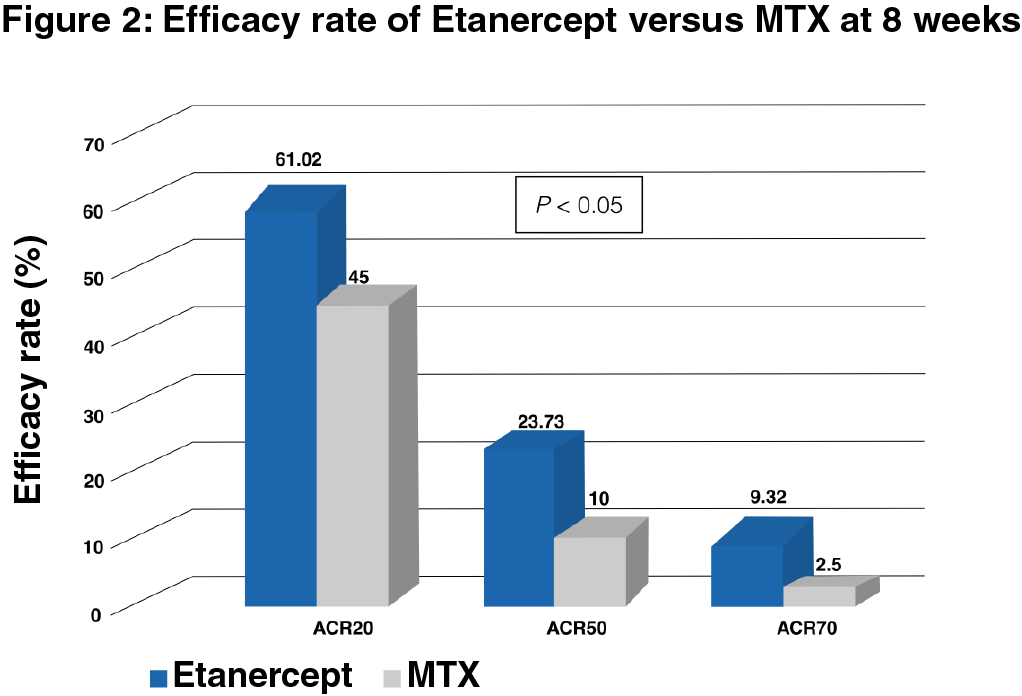
At 8 weeks
The efficacy rate of ACR20, ACR50 and ACR70 of the Etanercept group was significantly superior to the MTX group (P < 0.05), thus indicating Etanercept to be more effective at 8 week than MTX (Figure 2).
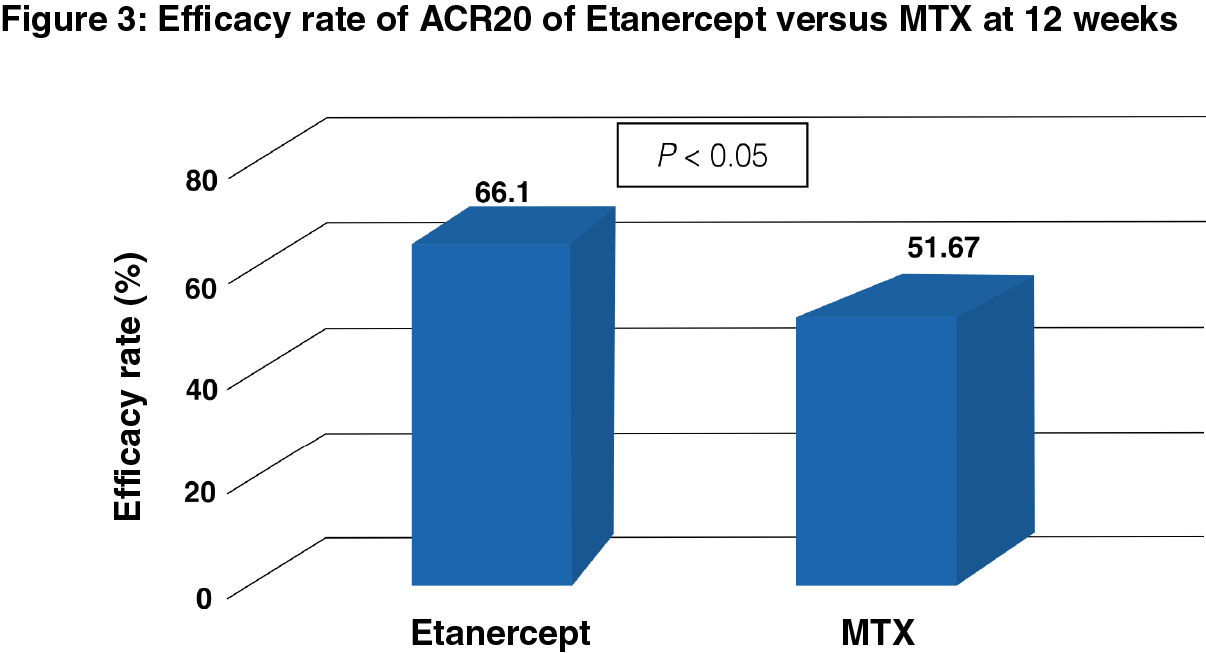
At 12 weeks
There was a significant difference in the efficacy rate of ACR20 of Etanercept and MTX (66.10% and 51.67%, respectively, P < 0.05) after 12 weeks treatment (Figure 3).
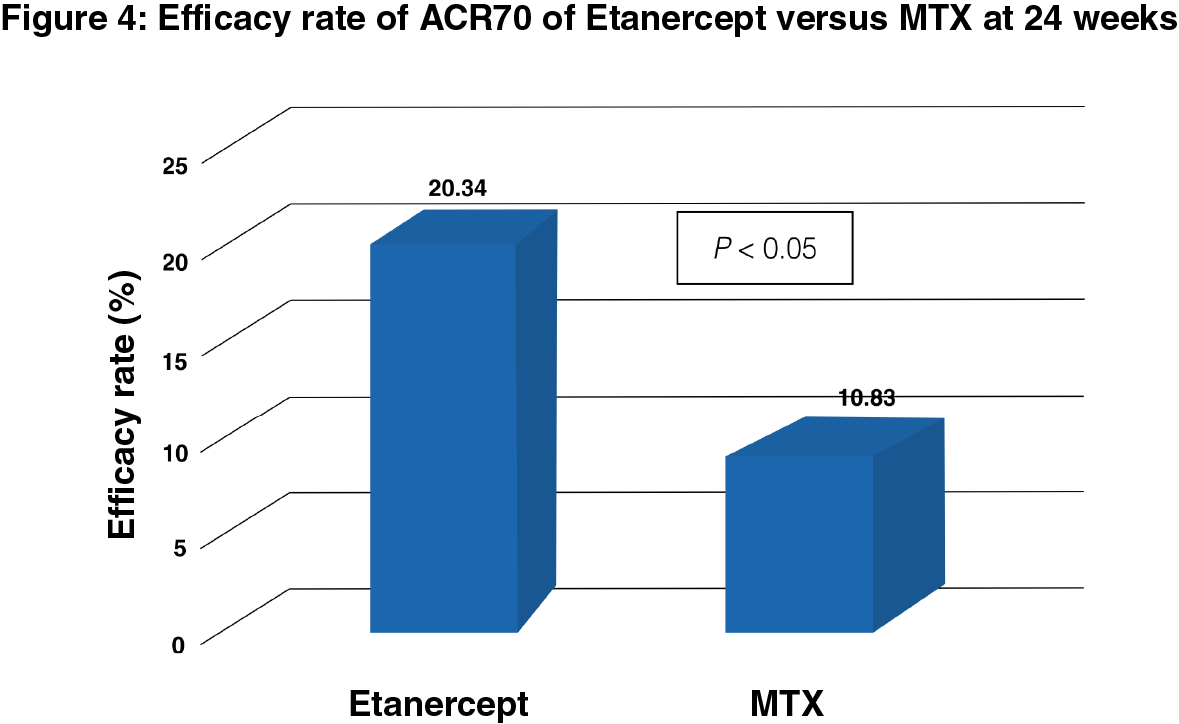
At 24 weeks
There was no difference observed in groups with ACR20 and ACR50 criteria. The ACR70 efficacy rate was found to be 20.34% and 10.83% for the Etanercept and MTX groups (P < 0.05), respectively (Figure 4).
Conclusion
The results demonstrated similar effects of Etanercept to that of MTX. Etanercept was superior to MTX both in quick responding and superior efficacy during the first 12 weeks of treatment. However, the study concluded that Etanercept has good safety and efficacy profile in the treatment of moderate and severe Rheumatoid Arthritis.
Reference:
Dawei Hu. Study 301-024 phase II clinical study report of ehTNFR: Fc in treatment of rheumatoid arthritis. NA: NA, 2004. NA.